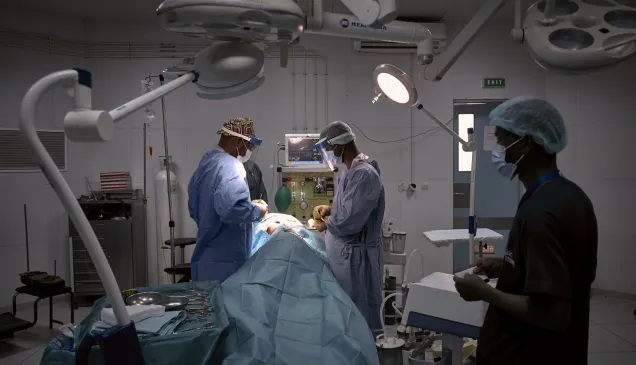
How ICRC-supported hospital in Mopti responded to COVID-19 pandemic

How the ICRC-supported hospital in Mopti responded to the COVID-19 pandemic: an interview with Shabani Majaliwa, anaesthesiologist
Shabani Majaliwa has been working as an anesthesiologist for the ICRC since 2015. His origins are from Congo, but he was born and raised in Burundi. From the start of his career in the ICRC, Shabani has worked in different contexts, each one of them with different challenges: in the Central African Republic, in Nigeria, in South Sudan, and finally in Mali where he has been working for the last three years.
He is now on a mission to support the ICRC hospital project in Mopti. We wanted to know how the COVID-19 pandemic has influenced or changed the management of the local hospital supported by the ICRC.

Could you give us an insight into the project, its main achievements and challenges before the beginning of the Covid-19 crisis?
"The ICRC came to Mopti in April 2019, to support the local hospital Somine Dolo, and provide assistance with the management of weapon-wounded patients in armed conflicts. Our support is mainly oriented on three axes: capacity building and management of weapon-wounded patients, provision of materials and consumables, and support in human resources, with mobile and resident staff.
The ICRC hospital team in Mopti consists of a hospital project manager, an anaesthesiologist, a mobile nurse and a surgeon, who is a local surgeon from Mali, a physiotherapist, and three nurses who are ICRC national staff. The hospital has fifteen surgeon specialists. One of the challenges is that the hospital has only two operation rooms, and at the same time lacks trained anaesthesia doctors, so we have to make queues for emergency cases.
Anaesthesiologists are indispensable to ensure that anaesthesia is provided in a safe way, and we only have two specialists, one hospital anesthesiologist, and the one from the ICRC team.
Since the start of the project, the total number of patients treated and discharged from the hospital was 831. Since the beginning of this year, 442 weapon-wounded patients have been treated and discharged. This has been possible due to a good collaboration and confidence installed between the ICRC and the local hospital staff.
The remaining challenge today for us is working in a volatile environment, especially during the pandemic of the COVID-19 and with no reliable curative treatment up to now."
When the COVID-19 first appeared in Mopti, what were the adaptions you had to make to successfully respond to the COVID-19 crisis?
"The COVID-19 outbreak, an emergency by itself, really had a potential risk to disrupt the whole organisation of our hospital. So, very quickly we had to adapt to the situation. Since 80 % of our patients come as an emergency, in a life-threatening condition that requires a prompt surgery, there is no room to reschedule the surgery or to postpone the treatment. So, we had to proactively make all possible efforts to adapt and deploy strategies to fight the pandemic.
We needed to deploy manpower for the COVID treatment area and increase protection, especially in terms of the personal protection equipment (PPE) and hygiene products delivered to the hospital.
We delivered teaching sessions about the COVID-19 to all our staff. We did a lot of simulation, for instance, for donning and doffing, which was quite new for some staff. We set up new patient circuits and triage zones.
This included checking the temperature of all patients and visitors at the entrance of the hospital and the provision of hand sanitizers. Ambulance patients needed to be checked up before getting out of the ambulance. In case a patient is suspected of COVID-19 infection, they are taken to the COVID treatment area.
One of the major concerns was to have our staff quarantined. For every staff infected, we had to put in quarantine all staff who had been in contact with this colleague, so there was a risk of lack of human resources. Some of the hospital staff and doctors were unfortunately infected, and we had a number of them in quarantine, but we managed to avoid any impact or disruptions in the health care provided to our beneficiaries. We had severe hygiene measures and wearing masks was obligatory for all the staff, patients and visitors to the hospital.
The biggest number of patients we had in the COVID treatment centre was around 15. Today, the number of infected patients has decreased significantly, for the last two months we didn't have any new cases. The staff is therefore again deployed in their initial positions in the hospital.
We also carried out some training beyond the Mopti project, by teaching a group of around 20 doctors in Bamako about the use of bedside lung ultrasound, a new technique in the management of COVID-19 patients in intensive care. As a result of this ICRC initiative, the Ministry of Health in Mali provided two ultrasounds for the Centre Hospitalier Universitaire du Point G, a teaching hospital in Bamako, dedicated to COVID intensive care."

What are the lessons you learned from facing the pandemic?
"It is really impressive how resilient we can be if we place the human in the centre of our concerns. It is very challenging to work in a conflict zone while facing the pandemic and staying for a long time away from our family. But the war-wounded need our help, and this is what makes us resilient.
Also, the proactivity of the ICRC, especially in terms of provision of the necessary PPE without any shortage, was something that prevented us from facing a disaster scenario here in Mopti. The local hospital staff is very grateful for the ICRC support during these times. They were in a very bad situation, but thanks to the ICRC, they managed to improve the quality of patient care."
Anesthesiologists have a crucial role in the treatment of COVID-19 patients, haven't they?
"Yes, because all the critical patients have to be handled by an anesthesiologist. In terms of diagnosis, the medical team also relies on his expertise. Here in Mopti, the one responsible for the COVID treatment area is the hospital anesthesiologist. Secondly, as in a cascade, we also help other intensivists. When it comes to suspected or confirmed COVID-19 patients requiring anaesthesia or requiring surgery, not only the anesthesiologist is highly exposed, he also has to work in a way to reduce exposure of other staff in the operation theatre. "
Training for regional anaesthesia with ultrasound in Mopti
In most of the low and middle-income countries, 80% of anaesthesia is usually provided by a nurse anaesthetist who doesn't have a formal diploma in anaesthesia. Recognising the need for capacity building, the ICRC team in Mopti has conducted training in regional anaesthesia using ultrasound, which is a quite new technique in Mali.
"We are the only organisation here providing these kinds of training up to now. Today, our nurses in Mopti manage to do the regional anaesthesia with ultrasound independently. We also provide training regarding difficult intubation and have started a similar capacity training project in Gao", said Shabani Majaliwa.