Yemen: The hardest part of being a doctor

A physician on the front lines in Yemen tells us about the stigma attached to working with COVID-19 patients, violence against health care services and personnel, and the importance of trust between health-care providers and the communities they serve.
"It shocked us all – people couldn't believe what was happening," Dr Abobakr said of last spring.
Aden's hot climate meant that illnesses such as malaria, dengue, cholera were already prevalent. Then COVID-19 added a massive challenge at a time when the medical community already had its hands full.
"We were looking towards other countries with far more means, and we saw that they couldn't manage to contain the virus, that people were dying in large numbers in Asia, in Europe. So, you can imagine how worried we were here in Yemen, which has a broken health system and a brutal war going on at the same time. It was all a bit overwhelming – as if living through war was not enough already," Dr Abobakr said.
The arrival of the pandemic came at the worst possible time. Yemen's health-care system had been broken by six years of unrelenting war. The fighting had destroyed much of the health infrastructure, disrupted medical supply chains and curbed the delivery of essential services. It had also led to an exodus of foreign medical staff, who had made up a significant proportion of the country's health-care professionals prior to the war.
There was little testing capacity in Yemen at the outset of the pandemic, and the disruptions caused by the conflict made implementing complex public health measures, such as effective quarantine procedures or contact tracing, nearly impossible.
By the end of July, the health authorities had recorded 1,726 confirmed cases and 487 deaths from COVID-19, one of the highest mortality rates in the world.

Sa’ada, Yemen. Children play football against a backdrop of destroyed houses, 2019.
"And then there is the fear of the virus, which at the beginning was so great, you cannot imagine. There were many rumours circulating at the time," Dr Abobakr said.
Rumours and conspiracy theories around COVID-19 have flared around the world, including in Yemen. Born out of fear and mistrust of official narratives about the virus's origins and contagiousness, misinformation and disinformation often overwhelmed and drown out official communications by health authorities.
Health-care workers protect us.
Yet in the past 5 years alone, we counted thousands of attacks on doctors, nurses, patients, hospitals, and more.
We are not doing enough to protect them. pic.twitter.com/wqzx7QuwoC— ICRC (@ICRC) May 3, 2021
Misinformation continues to sow confusion among those looking for trustworthy sources in an overwhelming amount of information, something that is particularly true in conflict settings where authority is contested and the health system tends to be weak.
Rumours also continue to drive violence against doctors and nurses, patients, hospitals and ambulances. These falsehoods paint health-care professionals as being involved in schemes to profit off the virus at the expense of patients or as being responsible for spreading the virus because of their proximity to patients.
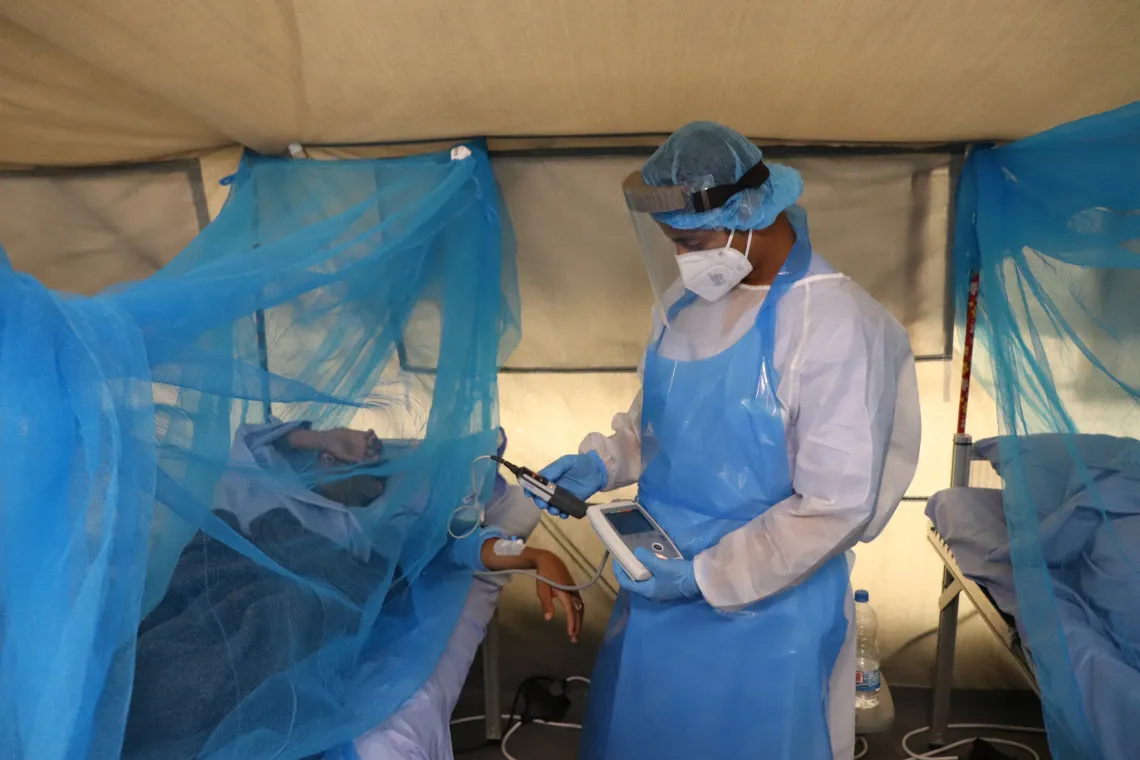
Aden, Yemen. Health staff at the Red Cross COVID-19 Care Center checking oxygen levels of a patient, November 2020.

Does it bother me that I am sometimes treated more like a COVID-19 case than a COVID-19 doctor? Yes, it does, but I understand where it comes from because people see me spend a lot of time in hospital with COVID-19 patients. The stigma that comes with this job is one thing – I have got used to it. But being attacked for my work, this I cannot accept.
Dr Abobakr
From February through December 2020, ICRC delegations in 42 countries received 848 reports of violence against health care linked to COVID-19, spanning the globe from Europe to Africa, the Americas and Asia.
Most attacks targeted health-care personnel and were generally perpetrated by state authorities, local communities or patients' relatives. The causes were varied and occurred all along the continuum of care: some objected to preventive measures promoted by health authorities, elsewhere people opposed the idea of testing.

Sana’a, Yemen. A health worker disinfects a market street amid concerns over the spread of COVID-19, April 2020.
Communities in multiple locations violently objected to the creation of quarantine centres, and in others, tribes and families used violence to express disagreement with relatives being transferred into quarantine.
Some cases documented by ICRC field teams were caused by frustration at the quality of treatment COVID-19 patients received in hospitals, others by anger and despair among relatives when health-care staff were unable to save a loved one.
Finally, where patients succumbed to the virus, restrictions imposed on funerals and traditional rites and customs owing to concern that they might contribute to spreading the disease also repeatedly provided a trigger for violent events.
Read the rest of Dr Abobakr's account along with other stories of hardships, resilience and change in times of COVID-19.



