“An emergency within an emergency” – Red Cross nurses on conflict and COVID-19
What does it mean to be a nurse today? We asked four nurses to share their experiences and explain how COVID-19 is impacting their work.
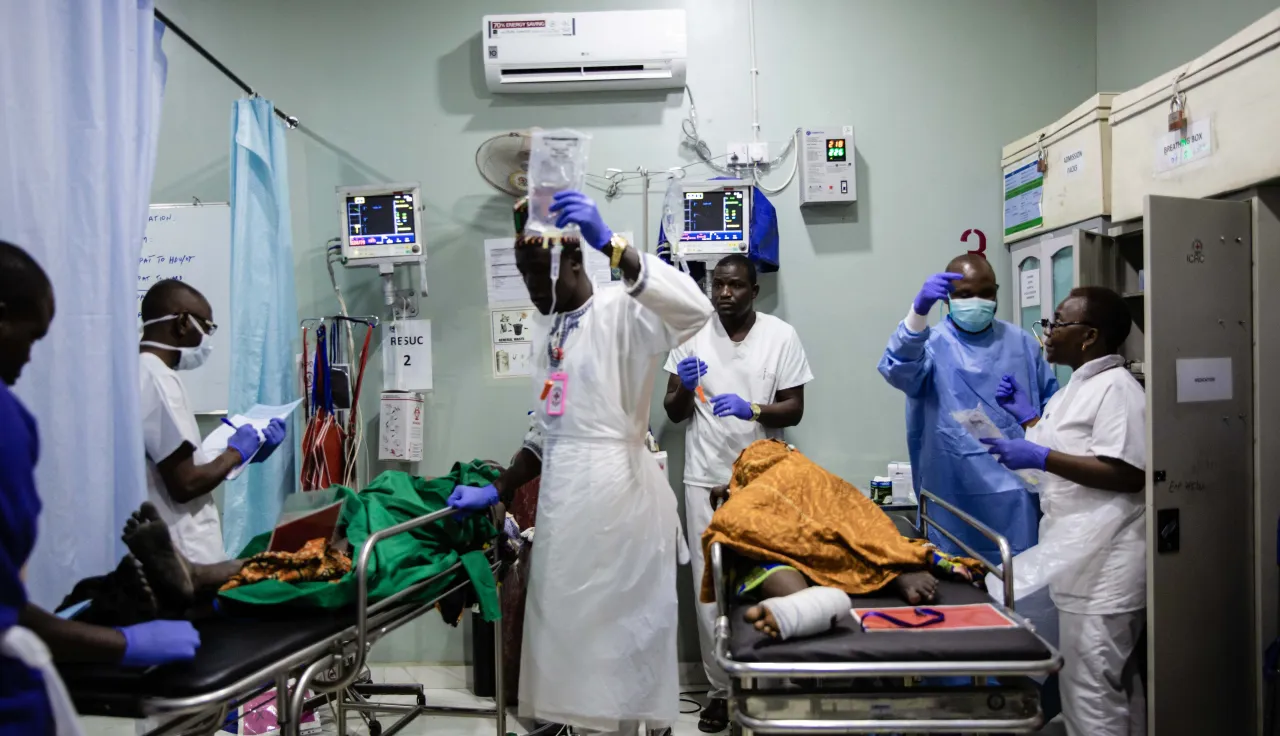
Natasha Moon, head nurse, Maiduguri, Nigeria
We're an emergency within an emergency: working in a conflict zone and now facing a massive public health crisis.
I'm based in the main Maiduguri hospital as part of an ICRC surgical team comprising international and local staff. Our remit is to treat people wounded by the conflict that has been raging for more than 10 years in north-east Nigeria.
The fighting hasn't stopped for coronavirus.
We still get mass influxes of patients following an attack or a spike in fighting. What's changed is how we deal with the situation.
We've set up triage tents and are training staff on prevention measures. We've also had to change our admission criteria. We're only admitting people into the emergency ward whose lives are in danger, or if they're at risk of losing a limb.
We've got social distancing measures in place and we've tried to free-up space on the wards to minimise contact. That's easier said than done. The hospital is a very busy place.
Maiduguri is home to around 3.5 million people, including over 1 million people who have sought refuge in the city having been uprooted by conflict.
They live in crowded camps dotted around the city, or within communities. The hospital is one of the few places they can get health care.

Natasha Moon works at the main hospital in Maiduguri. Alyona SYNENKO/ICRC
When I'm not with the ICRC, I work in NHS intensive treatment units back in the UK. I think you can make parallels between what we're doing here and the work of my NHS colleagues at home.
We're all delivering patient care to the best of our ability in difficult circumstances. As health-care professionals you are more vulnerable. You understand the risks and you willingly take those risks.
Coronavirus is an unknown to everybody, so it's more important than ever that we're there for our patients. That's the same whether you're a nurse in Maiduguri or in the UK.
If I was at home I'd be going to work with my team, doing my best for my patients, empowering the staff around me and supporting them. That's exactly what we're doing here.
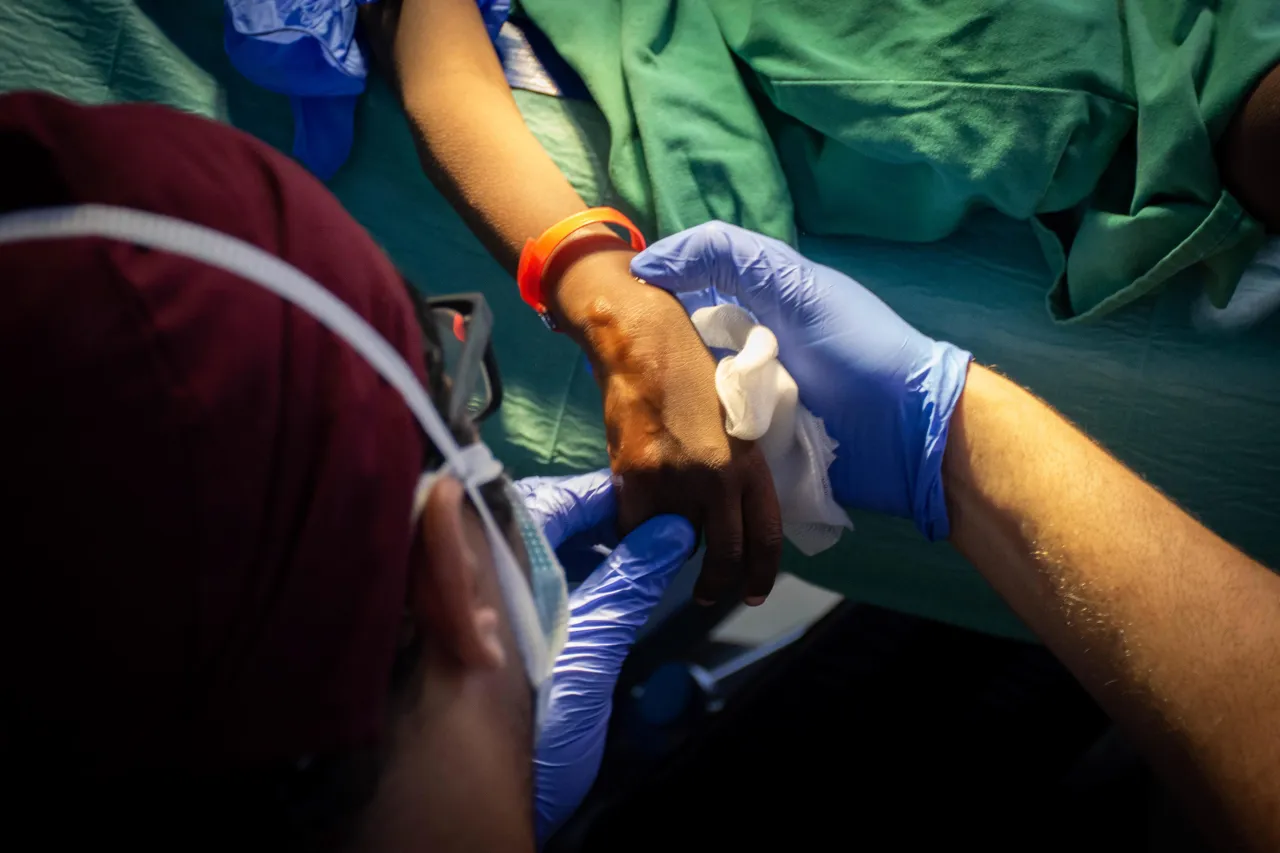
A young boy undergoes surgery in Maiduguri. Access to health care is difficult in north-east Nigeria. Sam SMITH/ICRC
Angela Neville, theatre nurse, South Sudan
As a nurse, you do your utmost to look after people who are at their most vulnerable. That doesn't change, no matter where in the world you're working.
What changes are the decisions you have to make.
I'm just back from South Sudan, where I was part of the surgical team at an ICRC hospital in a remote village in the heart of the world's newest country.
It's only accessible by plane or helicopter. In the wet season, sometimes even the helicopter can't land due to the mud, so you can become completely cut off.

Rainy season in South Sudan comes with challenges. Angela NEVILLE/ICRC
Unfortunately, conflict and intercommunal violence have blighted South Sudan's early years. We treat people suffering the effects of this violence.
You never get accustomed to helping people with gunshot wounds – the wounds we see are so different to anything back in our everyday life.
After a spike in fighting we would get a sudden surge of casualties coming to the hospital, all with gunshot wounds and other serious injuries. It gets very intense.
This is when you have to make critical decisions quickly. With the limited resources available, the decisions can be very difficult. Sometimes you think afterwards whether you made the right decision, you question yourself.
I know the choices I make in South Sudan are very different to those I'd make at my old London hospital, purely based on the resources we have available.
We're incredibly worried about COVID-19 in South Sudan.
The health system is already struggling. There are only four ventilators in the whole of the country. It just doesn't have the facilities, medical supplies or personnel, to cope.
Then you have to consider the huge number of people – around 1.5 million – who have been uprooted from their homes due to conflict. They face a battle to access clean water, soap, food and medical care as it is.
Beyond the medical factors, there are other issues that make the life of a nurse in South Sudan slightly more interesting. The heat – you get temperatures in excess of 50 degrees in the dry season.
We also have to contend with snakes and scorpions. On one of my previous missions, we were treating a patient who'd been brought to the hospital with a snake bite.
She was lying on the bed when she started pointing up at the ceiling – there was a green mamba right above her! It definitely made for an interesting start to the day.
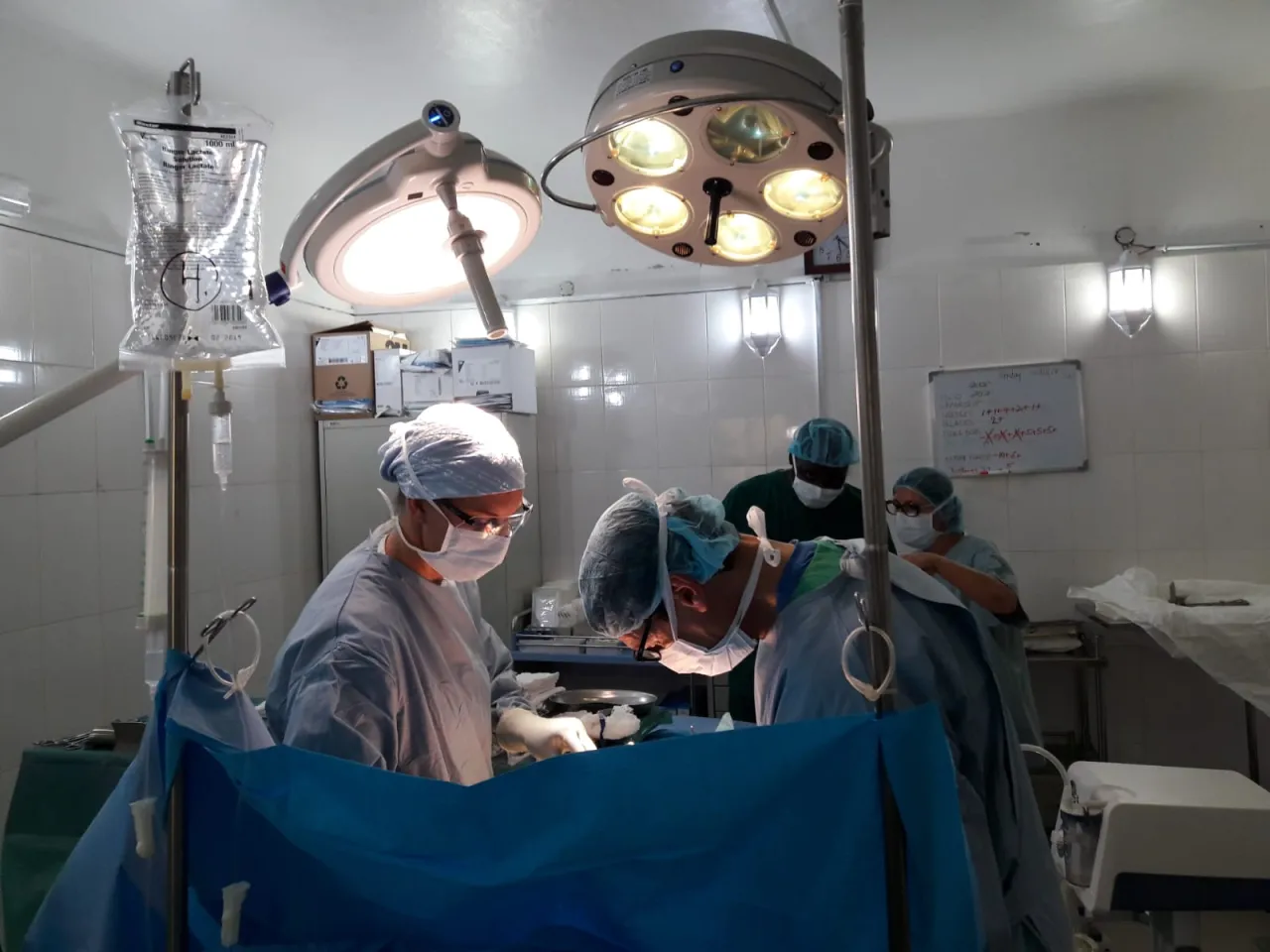
Making critical decisions quickly. Angela in surgery. Angela NEVILLE/ICRC
Frances Devlin, health coordinator, Damascus, Syria
Syria has entered its 10th year of conflict. A huge number of health facilities have been destroyed in the fighting. It's a major issue in restricting people's access to health care. Throw in a public health emergency and things become much worse. It is very worrying.
The provision of health care differs significantly across Syria. There's an ongoing conflict in and around Idlib, so there are acute health needs and limited access to health-care facilities.
There are an estimated 6.5 million people displaced within Syria, usually living in camps or in shared accommodation.
Take the Al Hol camp, in the north-east, as an example. You've got around 65,000 people living in close proximity. The tents often house multiple families, so it would be really difficult for people to self-isolate.

Two of Al Hol's younger residents. Mari Aftret Mørtvedt/ICRC
Working with partners, we're in the process of setting up an isolation centre in the camp. This will mean that suspected or confirmed COVID-19 cases can be isolated away from the densely populated camp.
But even then, it will be difficult for people with the virus to receive further medical treatment – leaving the camp to get to the hospital in Hasakah is no mean feat.
The ICRC is supporting a number of health facilities across the country with medical supplies and equipment. In addition, one of our main areas of focus at the moment is training medical staff.
In public health emergencies it's vital for their own safety and the patient's wellbeing that they know how to use personal protective equipment and how to triage patients properly.
It's the basics, but in a country where a lot of experienced medical workers have moved away, those left behind may not always have the necessary skills.
When I see how the world is responding to COVID-19, it's striking to see the outpouring of affection for nurses and medical personnel – whether at home in Ireland or anywhere else.
There's definitely a sense of pride in belonging to that nursing fraternity. Nurses are front line every day, not just for COVID-19. It's nice to see them finally getting the recognition they deserve.
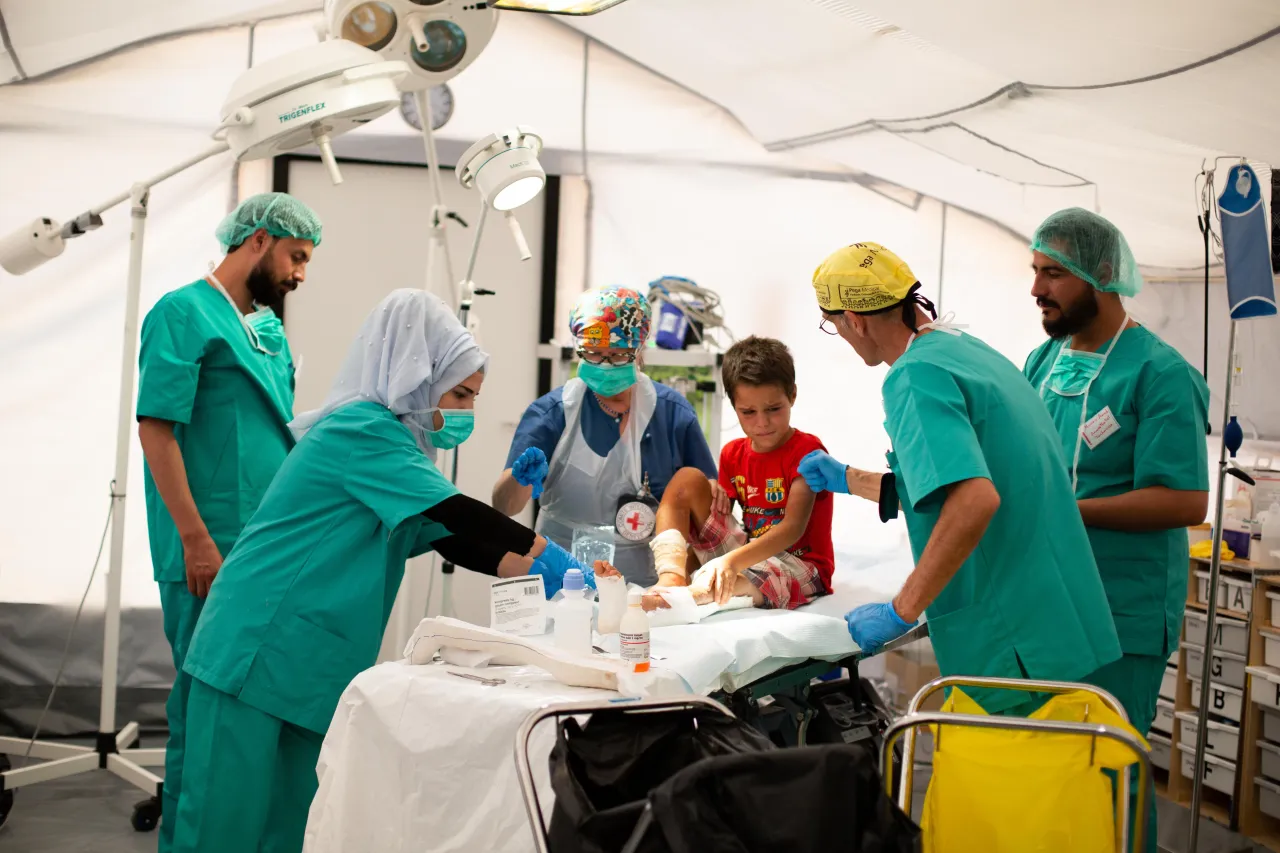
The ICRC runs a field hospital with the Syrian Arab Red Crescent in Al Hol. Mari Aftret Mørtvedt/ICRC
Chrissy Alcock, emergency nurse specialist, Caracas, Venezuela
I was in Sierra Leone in 2015 during the Ebola epidemic and in Bangladesh tackling the diphtheria outbreak among refugees from Rakhine State in 2018. It's very difficult to compare either context with what we're facing right now with coronavirus.
At the moment, we're not seeing a high number of coronavirus cases coming through the doors of the hospital that ICRC supports in Caracas – but that doesn't mean there aren't cases in the community.
It's very difficult to predict what's going to happen, so we have to use this time to prepare for the worst-case scenario. I'm part of a team helping to get the hospital ready for a potential surge in COVID-19 cases.
We're training hospital personnel in the use of personal protective equipment, looking at the hospital's triage system, identifying spaces to manage the patient flow and getting medical supplies and equipment ready. We're doing all this on top of the 'business as usual' work of the hospital.
Life is difficult for people in Venezuela. Although the country has one of the world's largest oil reserves, hyperinflation has reached significant levels leaving much of the population without access to food, adequate medical care and employment.
Chronic violence continues to affect some parts of the country while it's not easy for hospitals to get consistent supplies of water, electricity, medicine and health staff to ensure full functionality.
The migration of people out of Venezuela is well documented. What we find is that this leaves junior medical and nursing staff in positions that would normally be occupied by people with greater experience.
Part of my role is to train clinicians in emergency trauma. We also train the wider hospital staff in how to respond and behave during this pandemic.
We're all part of one team – the cleaner is just as important as the doctor.
There is a real camaraderie here and in the nursing community across the world. I used to work at St Thomas' hospital in London. I still feel part of the family there.
It's really sad when you hear about health-care staff who have died responding to this outbreak. We put ourselves in harm's way to treat patients.
In this International Year of the Nurse and Midwife I would like to pay tribute to the work of all my nursing and midwifery colleagues around the world.



